$11,000,000
Medical Malpractice
$8,000,000
Medical Malpractice
$5,200,000
Mother’s Wrongful death
Upstate New York Medical Malpractice Lawyers
We achieve life-changing results. Powers & Santola has long been recognized by “U.S. News and World Report" and "Best Lawyers in America” as one of America’s best medical malpractice law and personal injury firms. Best Lawyers in America is the most trusted and relied upon guide to legal excellence. Our relentless search for the truth has repeatedly earned our experienced lawyers recognition as Medical Malpractice Lawyer of the Year and Personal Injury Lawyer of the Year.
Learn More What Real Clients
Say About Powers & Santola
Read More Reviews ★★★★★
My experiences with Powers
& Santola were always positive.
Dan Santola helped guide my family through a difficult time and process with the highest sense of compassion and knowledge. Dan’s reputation in his field was evident. When I told other lawyers (both friends and business contacts) that we were working with Powers & Santola, we always hear in response – ‘Oh, they are by far the best in the state.’
★★★★★
It was not a long drawn out affair!
I highly recommend this firm
As an injured client, the team at Powers & Santola explained the legal process in a friendly manner that I could understand. In court, they were very professional. After, they helped in obtaining health insurance and information on handling my settlement. They had a very friendly and caring team, even after the case was done. Oh yeah, they are fast.
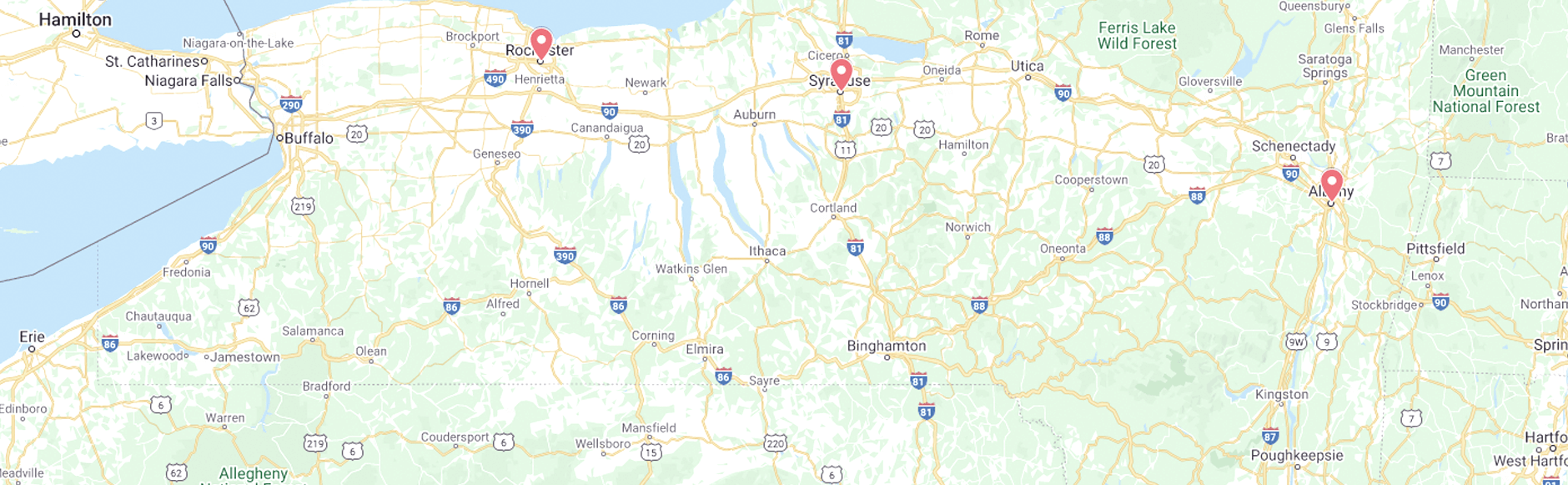
Powers & Santola Serves Seriously Injured People Throughout Upstate And Western New York
With offices in Albany, Syracuse, and Rochester, Powers & Santola provides local service to seriously injured individuals and their families throughout Upstate and Western New York.

Skill
Resources
We accept only a limited number of cases. There’s a reason for that: We want to make sure that each client receives the full benefit of our resources and gets the personal attention they deserve.
Dedication
Experience
Reputation
Powers & Santola, serves clients throughout New York from our offices located in Albany, Syracuse, and Rochester. Contact us today for a free consultation. We want to hear about your case.
Don't wait. Get legal help today. Contact Us Now for a free consultation.
free Case EvaluationYOU ARE NOT ALONE We’re here to help you
Our legal team at Powers & Santola is here for you. When we work for you, we have one goal – to change your life for the better.
- Protect your rights
- Regain control of your future
- Obtain the full compensation you are due
![Section: video]()
![Section: video]()